Issue Age Rating
Issue Age-rated states are those in which you are “locked” in at the age at which you get your policy. For instance, if you get your policy at age 65, you will always be charged 65-year-old rates. The premium can still go up every year, not because of your age, but because of several other factors including companies’ claims loss ratio, inflation, and many other factors. We find that issue-age states tend to have higher nationally averaged premiums, but are much more stable over time. Issue age states are the most important in which to make an informed decision on which plan and company you choose. This is because if you decide to switch plans or companies at a later age, you will then pay the premiums to reflect that age and lose your previous issue age.
What States are Medicare Issue Age rated? They include Florida, Arizona, Georgia, and Missouri.
Attained Age Rating
Attained age-rated states are those in which the premium always reflects your age. As you age, your risk is greater, and your premiums reflect that risk. In these states, you will find that premiums start out low at age 65, but tend to go up 4% or more every year with the chance of having 2 rate increases in the same year. One increase for age and another increase for reasons outlined above. Attained age states make shopping around every year worth your while as you were never locked into an age-like issue age state. Some companies still vow to only give one rate increase per year. Be sure to ask your agent which companies those are.
Community Age Rating
Community age states are those that charge the same premium no matter your age or gender. A male at age 80 will pay the same premium as a female at age 65 for the same plan and company. Premiums tend to be higher than the national average in these states since the premium is weighted between all ages and genders.
What states offer a community age rating for Medicare supplement plans? They include Arkansas, Connecticut, Maine, Massachusetts, Minnesota, New York, Vermont, Washington, and Idaho as of 2022.
What is a Birthday Rule for Medicare Supplement Plans?
It means you can change your Medicare supplement plan without being asked to go through underwriting health questions near the time of your birthday month on an annual basis. It is an example of a Guaranteed Issue application.
As of 2022, these states have a Medicare Supplement Birthday Rule: California, Oregon, Idaho, Illinois, Louisiana, Missouri and Nevada.
This appointment is meant to alleviate any concerns and there is no-cost or obligation to make a change.
New birthday rule for Idaho Medicare Supplement plans
Effective March 1, 2022, Medicare Supplement policyholders in Idaho may change their insurance company and/or plan annually, regardless of health conditions, during a 63-day enrollment period beginning on the policyholder’s birthday. These policies would be considered Guaranteed Issue.
Oregon Birthday Rule
Annual Open Enrollment lasting 60 days, beginning 30 days before and ending 30 days after the applicant’s birthday, during which time an applicant may replace any standardized Medicare supplement policy with a policy of equal or lesser benefits. Coverage will not be made effective prior to the applicant’s birthday.
Missouri Birthday Rule
Applicant’s that terminate a Medicare supplement policy within 30 days of the annual policy anniversary date may obtain the same plan on a guaranteed issue basis form any issuer that offers that plan. This would include Medicare supplement and select plans. Applicant’s with existing Plans E, H, I and J (no longer available) can convert to one of the following Plans: A, B, C, F, High Deductible Plan F, K or L if available.
Nevada Birthday Rule
As of January 1, 2022, individuals enrolled in a Medicare supplement policy in Nevada may change their plan or insurer during an annual enrollment period of up to 60 days following the first day of their birthday month.
The new plan choice is limited to any Medicare supplement policy that offers benefits equal to or lesser than those provided by the current Medicare Supplement plan. (Examples: Plan F to Plan F, Plan F to Plan A, Plan G to Plan B.)
Applications must be submitted within 60 days from the first day of the applicant’s birthday month, and the chosen effective date must fall within 90 days from the first day of the applicant’s birthday month. (Example: If an applicant has a May 25 birthdate, the effective date must fall between May 1 and July 30.)
Illinois Birthday Rule
Starting January 1, 2022, individuals between 65 and 75 years old who have an existing Medicare supplement plan can choose a Medicare Supplement policy from the SAME carrier that offers benefits equal to or lesser than their existing plan for a period of at least 45 days from their birthday.
The chosen effective date must fall within the 90-day time period beginning on the applicant’s birthdate. (Example: If an applicant has a May 25 birthdate, the effective date must fall between May 25 and August 25.)
California Birthday Rule
Annual Open Enrollment lasting 60 days, beginning 30 days before and ending 30 days after the applicant’s birthday, during which time an applicant may replace any Medicare supplement policy with a policy of equal or lesser benefits. Coverage will not be made effective prior to the applicant’s birthday. Please include documentation verifying the Plan information and paid to date of the current coverage.
Medi-Cal replacement – Open Enrollment for 6 months from the loss of Medi-Cal after notice of loss of coverage. Also applies to individuals who now only qualify for Medi-Cal benefits with a share of cost and the client has certified at the time of application that he or she has not met the share of cost. Not available for individuals with end stage renal disease.
Louisana Birthday Rule
As of August 1, 2022, there is a new guaranteed issue window available for policyholders in Louisiana. As related to the guaranteed issue of Medicare supplement policies. Enacts R.S. 22:1112. Requires an annual Open Enrollment Period to begin on the birthday of an individual who has an existing Medicare supplement policy. Requires the annual Open Enrollment Period to last for 63 calendar days, during which time the individual may purchase any Medicare supplement policy offered in this state by the same insurer.
Provided that if during the annual open enrollment period, the individual purchases a standardized Medicare supplement policy identified by a plan letter that indicates benefits equal to or less than the benefits indicated by the plan letter of the individual’s previous Medicare supplement policy, the issuer of the chosen Medicare supplement policy is prohibited from denying or conditioning the issuance or effectiveness of the coverage, or discriminating in the pricing of the coverage due to the individual’s health status, claims experience, receipt of health care, or medical condition.
What is a Medicare Guaranteed Issued Policy?
It is a policy that a Medicare supplement carrier can approve without needing to approve the applicant’s health through an underwriting process.
Difference between an Open Enrollment Policy and a Guaranteed Issue Policy
Open Enrollment is a qualified time to enroll for newly eligible Medicare recipients, without being subjected to pre-existing conditions. Guaranteed Issue policies are granted outside of the initial enrollment period for those eligible to submit an application without needing to be underwritten.
What states have a Guaranteed Issue Policy that exceeds the Federal Minimum Standard?
The Medicare Birthday Rule application can be considered in some respects both an Open Enrollment and a Guaranteed Issue policy. Since it’s during an eligible time to switch each year, but at the same time, not the initial enrollment period when first enrolling in Medicare Part B. However, we will consider it strictly Open Enrollment.
Other examples of being eligible for Medicare Guaranteed Issue: There are many other Guaranteed Issue periods that are outside of the Birthday Rule. They include being involuntarily (sometimes voluntarily) disenrolled from creditable coverage through an employer or union plan. Your Medicare Advantage or Medicare Select plan stops providing you coverage or you leave your service area. You are within your first year of a Medicare Advantage plan and 65 years old and have a trial right to return to Medicare. Among other examples you can read on Medicare’s government website here: Guaranteed Issue Rights.
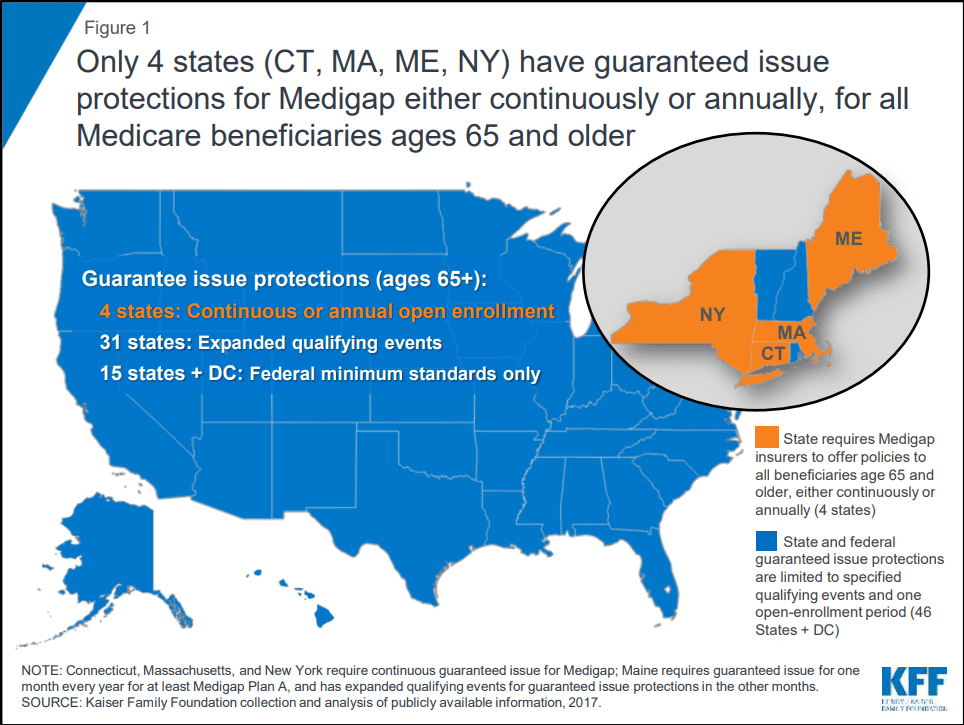
“Only four states (CT, MA, ME, NY) require either continuous or annual guaranteed issue protections for Medigap for all beneficiaries in traditional Medicare ages 65 and older, regardless of medical history. Guaranteed issue protections prohibit insurers from denying a Medigap policy to eligible applicants, including people with pre-existing conditions, such as diabetes and heart disease” – Keiser, 2018.
Conclusion
The rating class your state operates in has a major impact on the premiums of your policy and will give you great insight as to what to expect going forward with your Medicare Supplement. There are even rare occasions where a company could be community age-rated in an attained age state and vice versa.
